
Guest post: 10 climate-related events that cost the US $10bn in health impacts
Multiple Authors
09.18.19Multiple Authors
18.09.2019 | 6:00pmDr Vijay Limaye is a climate change and health science fellow at the Natural Resources Defense Council (NRDC) and Prof Wendy Max is a professor of health economics and co-director of the Institute for Health & Aging at the University of California, San Francisco (UCSF).
As the global climate movement turns to New York City this month for the United Nations Climate Action Summit, greater attention needs to be being paid to the increasingly visible costs to society from a warming climate.
Often, our understanding of these costs is limited to things we rebuild, insure, or repair, such as buildings, infrastructure, or damaged crops. However, that cost-benefit analysis often excludes the human health impacts of climate change.
Our research team at the Science Centre of the Natural Resources Defense Council (NRDC) – an environmental NGO – and the University of California, San Francisco (UCSF) today published a research article in the journal GeoHealth that sheds new light on the health costs of climate change in the US.
Our findings show that just 10 climate-related events in 2012 – from wildfires in Washington to Hurricane Sandy in New York and New Jersey – caused around $10bn of health-related costs to the US.
Public health risks
A warming climate brings a number of health risks to humans, from worsening heatwaves, disease outbreaks and scarce water supplies to increasing weather extremes, declining crop nutrition and impacts on mental health.
The costs of these impacts can be hard to estimate and have been largely absent from climate policy debates. For example, the “Billion-Dollar Weather and Climate Disasters” list, compiled by the US National Centers for Environmental Information (NCEI) each year, does not capture the economic impacts of health-related damages.
Our new study examines a set of US case study events from across the spectrum of “climate-sensitive” health hazards, such as extreme weather, heatwaves and increases in allergenic pollen.
While research attributing individual events to climate change has gained precision over time, attribution was not the focus of our case study selection. Rather, the “climate‐sensitive” case studies are characteristic of the types of health risks fuelled by climate change, to differing degrees.
The science tells us that the environmental exposures included in our analysis are each influenced by climate change and are expected to increase in frequency, intensity, duration, and/or a real extent in the future.
By linking health effect data with healthcare cost information, this work provides us with a new understanding of the present-day burden of climate-sensitive events on our health and the economy – and signals significant economic risks posed by climate change for the health sector.
Estimating health costs
Our analysis estimates illnesses and deaths related to climate-sensitive events and the associated costs of medical treatment and loss of life for 10 case studies occurring during the 2012 calendar year across the contiguous US.
The case study events we analysed spanned 11 states: wildfires in Colorado and Washington, harmful algal blooms in Florida, tick-borne Lyme disease in Michigan, Hurricane Sandy in New Jersey and New York, ozone air pollution in Nevada, allergenic oak pollen in North Carolina, extreme weather in Ohio, mosquito-borne West Nile Virus outbreak in Texas, and extreme heat in Wisconsin.
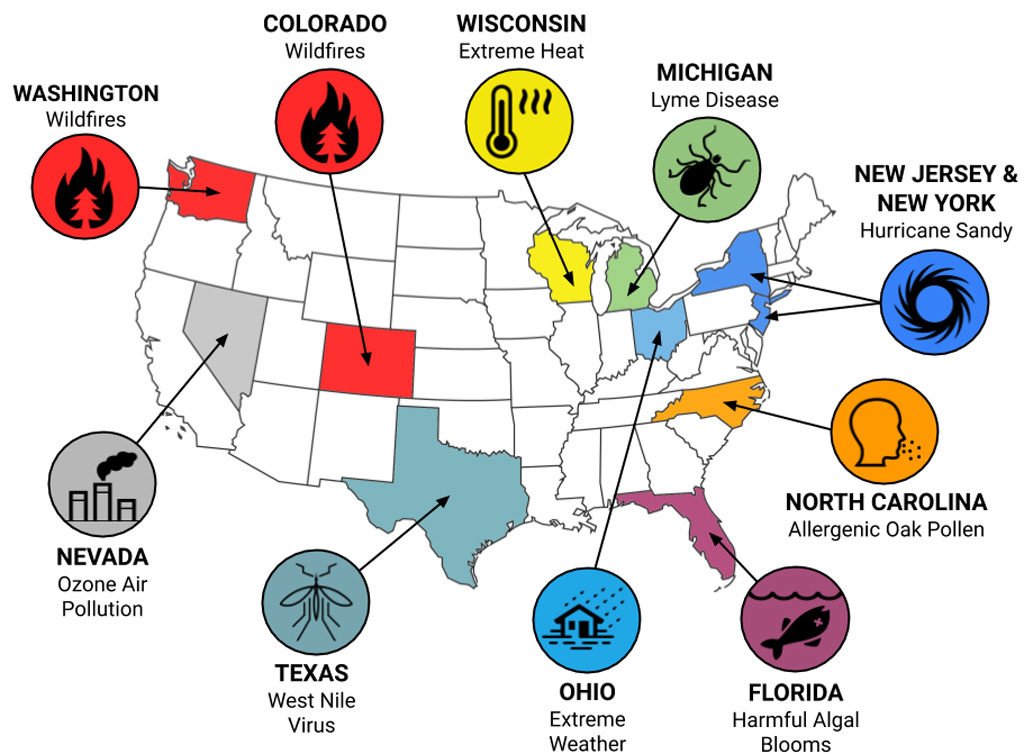
Ten climate‐sensitive case study events included in the health‐related cost valuation. Source: Limaye et al. (2019)
For each of these state-level case studies, our team analysed state-collected health surveillance data, federal reports, and other published data on the number of deaths, hospitalisations, and emergency room visits to calculate health-related costs.
Those costs include direct costs of lost lives and medical care, as well as expenses associated with lost wages, outpatient care and prescribed medications. We also estimated the impacts of these costs on a range of expected payers, including government-supported healthcare systems and private insurers. You see all the types of costs we included – and their data sources – in the figure below.
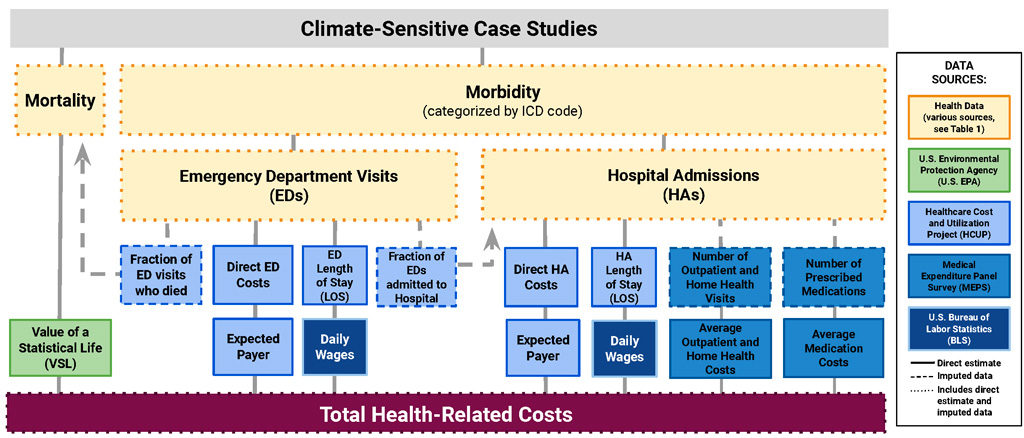
Data sources for health‐related cost estimates for all case studies. Solid lines are direct estimates, dashed lines are imputed data (inferred estimates from established ratios, such as the ratio of emergency department visits to hospital admissions), and dotted lines denote a combination of direct and imputed data. Source: Limaye et al. (2019)
Stitching together dozens of data sources, we estimated that the health costs of these 10 climate-sensitive events across the US in 2012 totalled $10bn (in 2018 dollars, see table below). These costs resulted from about 900 deaths, 21,000 hospitalisations and 18,000 emergency room visits.
We found that a disproportionate share of the illness-related costs of the events – about 64% – were expected to be paid for by Medicare and Medicaid, key taxpayer-funded health insurance systems. This imbalance aligns with our understanding that older adults and the economically disadvantaged are among those most vulnerable to the health effects of climate-sensitive events.
| State | Case study | Premature deaths | Hospital admissions | Emergency room visits | Total Health costs |
|---|---|---|---|---|---|
| Michigan | Lyme Disease | 0 | 157 | 11 | $8m |
| North Carolina | Allergenic Oak Pollen | 4 | 183 | 1149 | $43m |
| Ohio | Extreme Weather | 8 | 37 | 343 | $83m |
| Wisconsin | Extreme Heat | 27 | 155 | 1620 | $252m |
| Florida | Harmful Algal Blooms | 0 | 11066 | 3857 | $557m |
| Nevada | Ozone Air Pollution | 97 | 114 | 194 | $898m |
| Texas | West Nile Virus | 89 | 1628 | 2680 | $1.1bn |
| Colorado | Wildfires | 174 | 256 | 1432 | $1.6bn |
| Washington | Wildfires | 245 | 371 | 1897 | $2.3bn |
| New Jersey | Hurricane Sandy | 273* | 5795 | 2247 | $3.1bn |
| New York | 807 | 2426 | |||
| TOTAL | 917 | 20568 | 17857 | $10.0 billion | |
We note in our study that the total health-related costs of these events during 2012 could actually be as high as $25bn if we used the upper end of the mortality valuation methods used by the US federal government.
Broadening our understanding of climate damages
Our work suggests there have been, and will continue to be, hundreds of billions of dollars in health costs from climate-sensitive events in the US. And these costs are rarely discussed outside academic circles.
Our findings shows that these health costs are not only a future concern, they are already hitting vulnerable populations. These health effects have real consequences, both in individual pain and suffering and in financial and economic costs that are largely unaccounted for.
Some communities are more vulnerable to the ways that climate change negatively impacts our health, and others lack the economic capacity to prepare for and adapt to these effects. For example, in surveys from 2015-2017, 56% of US adults reported some kind of medical financial hardship trouble paying medical bills, worry about health costs, and/or delaying or foregoing treatment because of costs.
While the NCEI identified 11 disasters in 2012 that resulted in at least $1bn in property and/or infrastructure damages, the Federal Emergency Management Agency declared a total of 112 disasters that year and the number of annual billion dollar disasters was exceeded in 2016 (15), 2017 (16), and 2018 (14).
Since 2012, many additional weather records have been set across the country, and the world just experienced its hottest month on record in July 2019. The US has faced dramatic climate‐sensitive health episodes recently, including devastating hurricanes and 2018 wildfires in California that were the largest, costliest, and deadliest in the state’s history.
Adaptation strategies
While our study highlights another financial cost of our warming climate and the need for mitigation, it also emphasises the importance of adaptation.
Adaptation strategies that protect public health should become a priority at the local, state, regional, and national levels.
Some examples include employing heat early-warning systems and health-advice services, preparing public cooling centres, providing better disease surveillance, redesigning communities to withstand floods and storms, and reducing wildfire risks.
Only around a third of US states currently include public health measures in their climate change adaptation plans The US Centers for Disease Control and Prevention (CDC) runs programmes, such as the Climate-Ready States & Cities Initiative and National Environmental Public Health Tracking Network, which could be expanded with increased funding.
Our research illustrates the health costs of climate-sensitive events and shows that action on mitigation and adaptation together can help prevent unprecedented human suffering and major health-related costs – both right now and for years to come.

