
Guest post: Health benefits of Paris climate goals could save millions of lives by 2040

Guest authors
02.17.21
Guest authors
17.02.2021 | 12:50pmOn World Health Day in 2008, the World Health Organization (WHO) declared that “protecting human health is the ‘bottom line’ of climate change strategies”.
The WHO went on to describe climate change as “the biggest global health threat of the 21st century”. This is because – through its effects on food security, heatwaves, floods, storms, wildfires, infectious diseases, air quality, migration, conflict and mental health – climate change both exacerbates existing health threats and creates new ones.
At the same time, a Lancet Commission on health and climate change found that “tackling climate change could be the greatest global health opportunity of the 21st century”. Many efforts to mitigate and adapt to climate change also work towards tackling some of the world’s biggest health challenges in the form of non-communicable diseases.
This is good news, not only because of the opportunities to benefit health, but also because the evidence suggests that framing climate change in this way can help gain public support for stronger government action.
The health opportunity of more ambitious climate policies is the focus of our study, recently published in the Lancet Planetary Health. We take nine globally and regionally influential countries and model the potential health gains they could achieve if they had climate policies that were consistent with the goals of the Paris Agreement.
Our findings suggest that the co-benefits for reducing air pollution, improving diets and encouraging a more active lifestyle would save millions of lives across the world every year.
Health co-benefits of climate change mitigation
There are numerous ways in which efforts to tackle climate change can have a positive impact on public health. In this study, we focus on three.
First is avoided air pollution from reducing reliance on fossil fuels for energy. The WHO estimates that indoor and outdoor air pollution are together responsible for seven million deaths globally each year. And a recent study estimates that annual deaths due to emissions of fine particulate matter – known as “PM2.5” – from fossil fuel combustion could be as high as 8.7 million. Efforts to phase out fossil fuels will go a long way to reducing global deaths from air pollution.
Second is healthier diets. The Intergovernmental Panel on Climate Change (IPCC) estimates that 21-37% of total greenhouse gas emissions come from the food system. Diet-related risk factors – such as high salt intake and low consumption of fruit and whole grains – are also responsible for an estimated 11 million deaths each year. Diets that reduce red meat and dairy consumption and increase consumption of fruits, vegetables, legumes and nuts can help mitigate agricultural emissions and this global health burden.
And the third is a greater emphasis on “active travel”. Physical inactivity is another leading risk factor for death and disease. More than a third of adults in high-income countries do not achieve the recommended physical activity levels. Policies that promote active travel – such as walking and cycling – as main modes of transport for short trips could tackle land transport emissions and increase physical activity.
Potential health benefits of meeting the Paris Agreement
In our study, we model the annual health benefits in 2040 if nine countries adopted climate policies in line with International Energy Agency’s (IEA) “Sustainable Development Scenario” – referred to in our paper as a “Sustainable Pathways Scenario” (SPS) – compared with national climate policies as they stood in mid-2019.
The SPS describes a world in which global temperature rise is kept below 1.8C with a 66% probability, without reliance on global net-negative CO2 emissions. In keeping with the Paris Agreement, the SPS reaches “a balance between anthropogenic emissions by sources and removals by sinks (i.e. net-zero emissions) in the second half of this century”.
Alongside this we model changes in diet and active travel that would also be consistent with the SPS.
The nine countries – Brazil, China, Germany, India, Indonesia, Nigeria, South Africa, the UK and the US – represent more than 70% of global emissions and 50% of the global population.
Across these countries, we estimate that increasing ambition to be consistent with the Paris Agreement could result in an annual reduction of 1.18 million deaths due to air pollution, 5.86 million deaths due to diet-related risk factors, and 1.15 million deaths due to physical inactivity by 2040.
All countries benefit from the reduction of each of these different risk factors, with changes in diet yielding the greatest benefits in each. Considering deaths avoided per 100,000 population, the greatest gains could be seen in Indonesia, Germany and the US in terms of changes in air pollution, diet and active travel, respectively.
You can see this in the charts that follow, which shows the avoided deaths per 100,000 of population under the SPS scenario (and a second scenario, “HPS” – more on that below) for the nine countries under different policy shifts.
First up is air pollution, which shows the avoided deaths separated out into sectors of the economy.
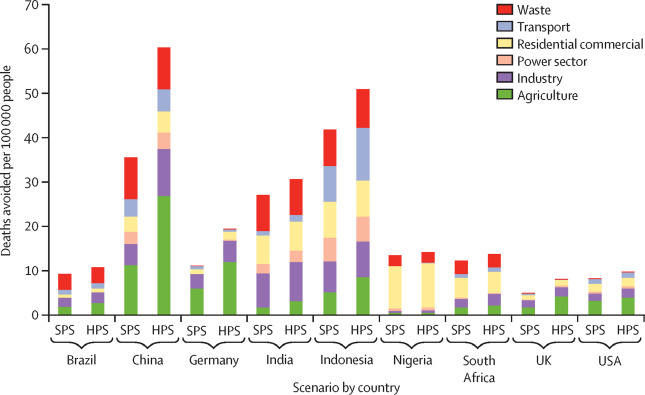
Taking the measures one step further, we modelled what would happen if the climate change and public health agendas aligned and if positive health outcomes became a key objective of climate change policies alongside reducing greenhouse gas emissions. We call this the “Health in all climate Policies Scenario” (HPS).
The second chart, below, shows the SPS and HPS results for deaths avoided thanks to healthier diets. Here, the bars are divided up by the specific dietary changes.
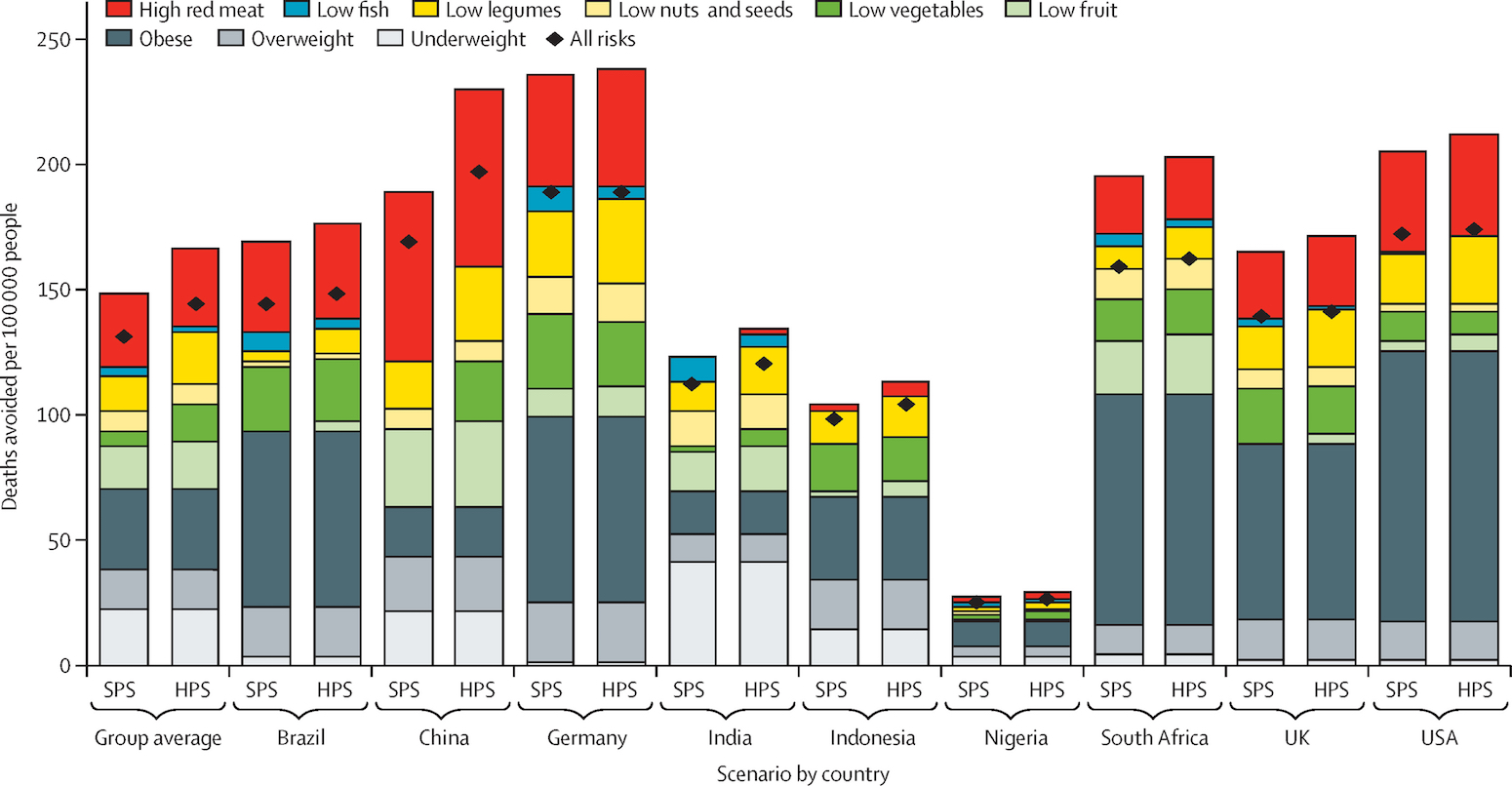
For air pollution under HPS, this meant the introduction of additional air pollutant emission controls. For diets, the shift was to a combination of flexitarian and plant-based diets. For active travel, we modelled the physical activity to reflect 75% of the population aged under 85 years in each country walking or cycling as a main mode of transport.
Compared with current pathways, these further changes could result in an annual reduction of 1.64 million air pollution-related deaths, 6.43 million diet-related deaths, and 2.08 million deaths due to physical inactivity, across the nine countries, by 2040.
While the changes may seem quite different to what we do today, these reflect the scale of the shifts we need to tackle non-communicable diseases as well as mitigate climate change.
The third and final chart, below, illustrates the avoided deaths from active transport in SPS (pink bars) and HPS (purple).
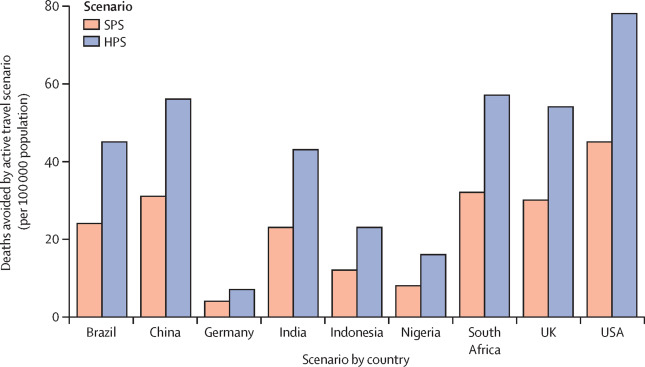
Aligning health and climate agendas
For much of the past 30 years, climate policy and health policy have been largely distinct areas, with efforts to reduce CO2 emissions globally and to improve public health taking place in separate departments in governments around the world.
Moving forward, health actors from around the world met at the Global Conference on Health Promotion in 2013, and announced the “Helsinki Statement” (pdf). This called for a policy approach across sectors that “systematically takes into account the health implications of decisions, seeks synergies, and avoids harmful health impacts in order to improve population health and health equity.” This approach is at the core of considering what the health co-benefits of action limiting global warming could be.
Aligning the policy objectives of health and climate change will likely yield greater societal and political buy-in. However, reframing the issue will, on its own, not be sufficient to limit global warming to acceptable levels.
In its latest Emissions Gap report, the UN Environment Programme (UNEP) finds that, even with a net-zero pledge from the new US administration, global temperature rise would be above 2.5C. This underscores the immense task that decarbonisation presents and the absolute necessity to get to work right away. The longer governments wait, the greater the delay will be in avoiding deaths.
Challenges
The full benefit of active lifestyles and clean air will require considerable co-ordination amongst policymakers and planners – not least to provide urban spaces with high-quality walking and cycling routes and accessible public transport.
The Covid-19 pandemic – and the resultant lock-downs imposed worldwide – have underscored the inadequacy of much of our built environment. Urban spaces suffer for a lack of access to green space and rural areas remain heavily reliant on cars.
These issues are compounded by social inequality – lower income communities face higher air pollution exposure and have much less access to the flexibility that allows higher income groups to work remotely in areas with lower pollution levels.
Related challenges are seen when addressing dietary change due to a complex entanglement of economic and social factors. The communities most at risk of poor health due to nutrient deficient diets lack the economic means to enact substantive change.
This pattern is seen both in developing nations – which will require substantial financial support from richer countries – but also within wealthier nations, such as the UK, where poor diet contributes to some of the substantially reduced life-expectancy seen in economically marginalised communities.
In the UK, action on this has taken the shape of a National Food Strategy, with the aim of delivering “safe, healthy, affordable food, regardless of where people live or how much they earn.” The findings of an initial consultation are due to be published in the coming months, but to what extent the urgency of action on the greenhouse emissions associated with food will be addressed remains to be seen.
As the world prepares to come together for the COP26 climate summit in November, it is clear further ambition is necessary from all governments to limit global temperature rise to 1.5C. Stronger climate policies could benefit the health of populations in every country, now and across this century.
Hamilton, I. et al. (2021) The public health implications of the Paris Agreement: a modelling study, The Lancet Planetary Health, doi:10.1016/S2542-5196(20)30249-7
-
Guest post: Health benefits of Paris climate goals could save millions of lives by 2040
-
Guest post: The health implications of the Paris Agreement

