Q&A: Could climate change and biodiversity loss raise the risk of pandemics?
Daisy Dunne
05.15.20Daisy Dunne
15.05.2020 | 8:00amAcross the world, millions of people have tested positive for Covid-19 – and countless more have seen their lifestyles completely transformed as a result of the virus.
It is not yet known exactly what triggered the current outbreak, but researchers suspect that the virus passed from bats to humans through an unknown intermediary animal, possibly a pangolin.
Politicians in the UK have called this pandemic a “once-in-a-century” crisis. But scientists have warned that the ongoing disturbance of species through human activities and climate change could be raising the risk of potentially pandemic-causing diseases passing from animals to humans.
The study of the “spillover” of disease from animals to humans has received renewed focus in light of the pandemic. The Intergovernmental Panel on Climate Change (IPCC) – a major international collaboration of climate scientists – is now looking into how the influence of warming on such events could be included in its next major climate report due next year.
In this explainer, Carbon Brief examines what is known about how climate change and biodiversity disturbance, including habitat loss and human-animal conflict, could influence the risk of diseases being transmitted from animals to humans.
- How does an animal-to-human disease spillover turn to a pandemic?
- Could climate change and biodiversity disturbance affect the risk of spillover?
- Will the risk of animal-borne disease pandemics increase in the future?
How does an animal-to-human disease spillover turn to a pandemic?
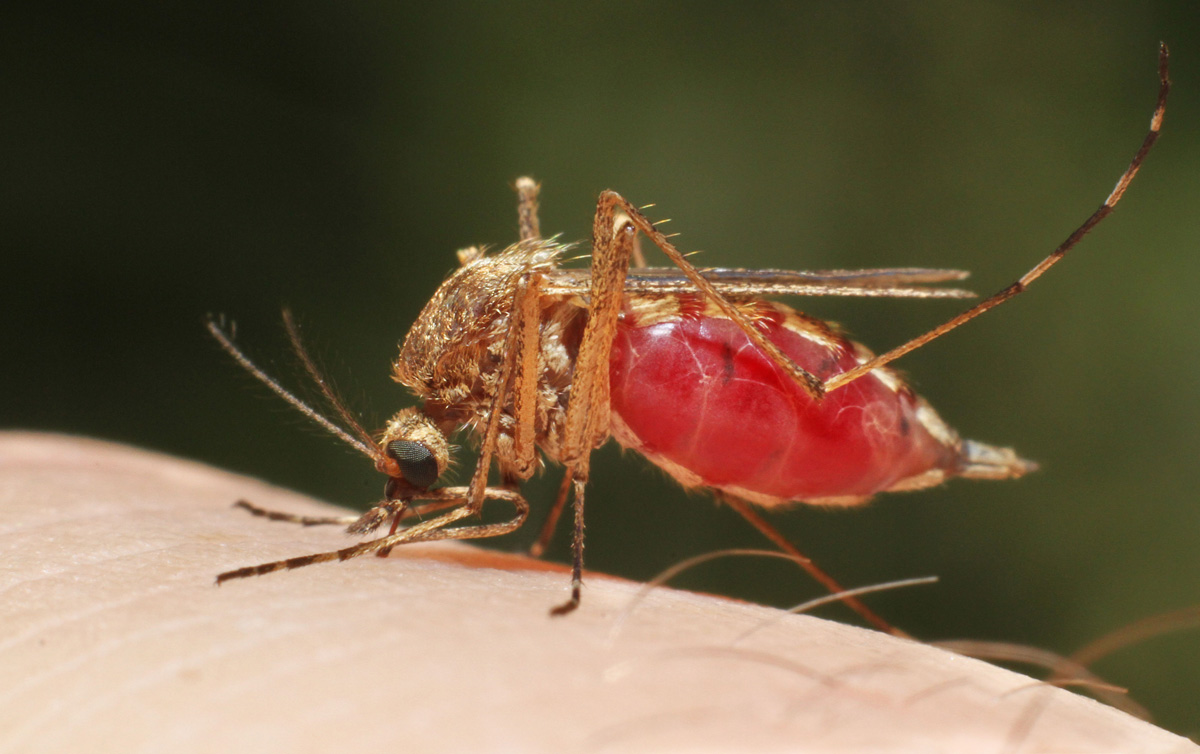
When humans come into contact with other animals, they can pass harmful pathogens between one another. The passing of an infection or disease from a vertebrate animal to a human is known as a “zoonosis”, according to the World Health Organisation (WHO). (Vertebrate animals include mammals, birds and reptiles, but not insects, such as mosquitoes.)
- IEA: ‘Green’ coronavirus recovery would keep global emissions below 2019 peak
- Coronavirus: Tracking how the world’s ‘green recovery’ plans aim to cut emissions
- Webinar: What impact is Covid-19 having on global CO2 emissions?
- Q&A: Could climate change and biodiversity loss raise the risk of pandemics?
- Analysis: Coronavirus set to cause largest ever annual fall in CO2 emissions
- Coronavirus: What could lifestyle changes mean for tackling climate change?
- Analysis: Coronavirus temporarily reduced China’s CO2 emissions by a quarter
Such diseases have a major impact on health, accounting for two-thirds of all human infectious diseases and three out of four newly emerging diseases.
Serious diseases that have spilled over from animals to humans include Ebola in Africa, Marburg in Europe (and subsequently in Africa), Hendra virus in Australia and severe acute respiratory syndrome (SARS) coronavirus and Nipah virus in east Asia. Some have gone on to have a lasting, global impact, such as HIV/AIDS and swine flu (H1N1). The current Covid-19 pandemic was also most likely caused by a spillover.
The number of potentially harmful viruses circulating in mammal and bird populations that have not yet spilled over to humans is estimated to be up to 1.7m, according to the Intergovernmental Science-Policy Platform on Biodiversity and Ecosystem Services (IPBES). (IPBES is an independent group of international researchers monitoring biodiversity issues).
The spillover of disease from animals to people can happen in many ways, including directly through animal bites, the consumption of raw or undercooked animal meat or products such as milk, or through contaminated water. Diseases can also spread indirectly if humans come into contact with a surface that has been contaminated by an infected animal. Both wild animals and livestock can pass on disease.
(Sometimes, transmission occurs through an intermediary species that can carry the disease without getting sick. Scientists suspect this is how the Covid-19 pandemic started.)
Out in the wild and in settings where humans and animals come into contact, these kinds of interactions happen regularly – and it is rare for one to end with a human being infected by a new disease, explains Dr David Redding, a research fellow at the Zoological Society of London. He tells Carbon Brief:
“There are lots of different factors that need to all overlap at the same time for there to be a contact that is both effective in terms of transferring a live pathogenic organism and then also for that very rare situation where that pathogen has an adaptation that allows it to invade our immune system.”
Even if a disease is effectively transmitted from an animal to a person, it is unlikely that they will then pass it on to someone else, he adds:
“I would say most – possibly 99% – of all diseases that are caused in that way can’t then be passed on. So we’ve got another ‘filter’ that dictates that people have to be infected in a particular way that allows them to shed viruses effectively to other people.”
This “virus shedding” can happen in various ways. Like other respiratory diseases, Covid-19 can be transmitted when a carrier coughs or sneezes in close proximity to another person. (Scientists are still debating whether the virus can also be passed on in other ways.)
The ability of the new pathogen to spread directly from person to person is a key ingredient for a disease to take hold in a population, Redding says. (Some animal-borne diseases require a vector to spread from person to person, such as West Nile virus and Lyme disease.)
An illness outbreak is said to become an “epidemic” when its impact on people in a single community or region is “clearly in excess of normal expectancy”, according to the WHO. The term “pandemic” describes the worldwide spread of a new disease. (When a disease is “endemic” it has a continuous presence in a population or area.)
Since 1900, there have been pandemics at “intervals of several decades”, according to the WHO. The worst in this time period was Spanish flu, which killed an estimated 50 million people from 1918-19.

Prior to Covid-19, every outbreak considered to be a pandemic by the WHO since 1900 has been caused by influenza, a virus that transmits from person to person. Some new strains of flu originate in animals, such as bird flu, but most new strains arise in human populations – and so would not be considered animal-borne.
There are many factors that can determine whether an outbreak reaches epidemic or pandemic status. These include human factors, such as preparedness and early action to prevent the illness from spreading, and also the traits of the pathogen itself, says Redding:
“The characteristics of the pathogen and its ability to spread are two key components in causing these rare events.”
For instance, if the pathogen causes very severe illness, the sufferer is less likely to be able to travel to a new place to pass on the disease, Redding says. This is also the case if the mortality rate is particularly high.
In contrast, if the disease causes mild to undetectable symptoms for at least some sufferers – as is the case with Covid-19 – it is more likely that people will inadvertently spread it to new places, he says.
This may go some way to explaining why previous serious animal-borne disease outbreaks have not reached pandemic status, Redding explains.

Members of a burial team prepare for a burial in Komende Luyama village. Eastern Sierra Leone was a hot spot for Ebola for several months, but eventually authorities managed to bring down infection rates to just a few cases per week. 17 October 2014 Credit: Tommy E Trenchard / Alamy Stock Photo
For example, Ebola – a disease initially spread to humans by fruit bats – has caused several serious epidemics in West Africa, but has not established itself on a worldwide scale. It has a mortality rate of around 50%. The mortality rate of Covid-19 is not yet known, though it is likely to be below 10%.
It is also worth noting that the likelihood of a disease turning to a pandemic has been heightened in recent decades by increased global connectivity, particularly through frequent air travel, Redding says:
“Plagues in the medieval times took years to spread across Asia. Whereas we look at today’s outbreaks and we can see that they can spread in hours.”
Overall, for a spillover event to turn into a pandemic, there must be a “perfect storm” of several complex factors all occurring at the same time – which, at present, does not happen very often, says Redding: “I think history shows us that these sort of large outbreaks happen a couple of times a century.”
Could climate change and biodiversity disturbance affect the risk of spillover?
Every new animal-borne disease starts with humans coming into contact with wildlife. And it is likely that climate change and the disturbance of biodiversity could play a role in shaping the frequency, timing and location of these meetings, says Prof Hans-Otto Poertner, head of biosciences at the Alfred Wegener Institute (AWI) and co-chair of the impacts chapter of the next major assessment report from the IPCC. He tells Carbon Brief:
“Climate change is clearly a factor that can influence these relationships. Climate change shapes the biogeographical distribution of species. If, in the future, we see species moving into areas where humans are prevalent, we could see new opportunities for pandemics to evolve.”
Research has shown that climate change is shifting where species live, both on land and in the ocean. This is because, as temperatures increase and rainfall levels change, some species are being forced to seek out new areas with climate conditions they are able to tolerate. (Species that are not able to adapt could face extinction.)
A review published in Science in 2017 looking into 40,000 species across the world found that around half are already on the move as a result of changing climate conditions.
In general, species are seeking cooler temperatures by moving towards the Earth’s poles. Land animals are moving polewards at an average rate of 10 miles per decade, whereas marine species are moving at a rate of 45 miles per decade, according to the review.

Dugong feeding in the seagrass bed, Dimakya Island, Palawan, Philippines. Credit: Nature Picture Library / Alamy Stock Photo
However, the movement of animals is complicated by other factors, such as the changing availability of food, the shifting distribution of predators and changing patterns of human land-use, the review says. This makes it difficult to predict exactly where species will move to.
It is likely that the movement of species will have consequences for human health, says Prof Birgitta Evengard, a senior researcher of infectious diseases at Umea University in Sweden, who was one of the authors of the review. She tells Carbon Brief:
“When land-based animals move, they bring with them their [viruses] – and they will spread them.”
So far, there has not been a great deal of research into how climate change-driven shifts to animal ranges could affect the chances of disease spillover on a global scale, says Poertner.
In one example, a research paper by Redding found that climate change could heighten the risk of new Ebola outbreaks in various parts of Africa by 2070.
This is because climate change could cause regions that are currently desert to become warmer and wetter, leading to the formation of the lush plants that bats use as a habitat. The movement of bats into these new areas could increase contact between them and humans, increasing the chances of disease spillover, the study found.

Another study found that climate change could enhance the risk of spillover of the Hendra virus, an animal-borne disease that can pass from flying foxes to humans through horses, which are also affected by the virus.
The virus was first identified when an outbreak broke out in Hendra, a suburb in Brisbane, Australia, in 1994. Since then, there have been at least eight separate outbreaks along the coast of northern Australia, according to the WHO. It has a mortality rate of 50-75%.

The research found that climate change could cause the geographic range of flying foxes to expand southwards and further inland. “Spillover events could potentially increase farther south, and inland with climate change,” the authors say.
Elsewhere, a recent preprint – a preliminary study that has not yet completed peer review – suggests that climate change could drive substantial global increases in the passing of novel diseases from mammals to humans by 2070.
Using modelling, the study maps where around 4,000 mammals species and the diseases they carry are likely to move to by 2070. It finds mammals are “predicted to aggregate at high elevations, in biodiversity hotspots, and in areas of high human population density in Asia and Africa, sharing novel viruses between 3,000 and 13,000 times”.
The authors add: “Most projected viral sharing is driven by diverse hyperreservoirs (rodents and bats) and large-bodied predators (carnivores).”
It will be important for the IPCC to include the emerging evidence of how climate change could affect the passing of diseases from animals to humans in its next major assessment report, currently due for release in 2021-22, says Poertner:
“We expect to include aspects as they become apparent from the literature.”
The scale of the impact of climate change on wildlife is currently second only to the damage caused by human land-use change, including deforestation, other types of habitat loss and human-animal conflict.
In its first major assessment on biodiversity published in May 2019, IPBES reported that humans have “significantly altered” 75% of the land surface and 66% of the global ocean. During 2010-15, 32m hectares of natural or recovering forest were cleared by humans. This area is roughly equal to the size of Italy.
As a result of ongoing pressures on biodiversity, around one million species are currently threatened by extinction within decades, the report concluded.
The report noted that ongoing pressures on wildlife are likely to increase contact between animals and humans, altering the chances of disease spillover. In chapter three of the full report, the authors say:
“Complex links between increased human disturbance, land-use change, habitat loss/degradation and biodiversity loss have all been linked to increases in the prevalence and risk of zoonotic [animal-borne] disease for a variety of pathogens.”
However, research into how biodiversity disturbance could affect animal-borne disease risk at a global level has so far been limited, it notes:
“Causal mechanisms are only well known for a handful of infectious diseases and it is sometimes hard to pick apart the drivers of disease to isolate the direct effects of environmental change from other human actions.”
Research has shown that bushmeat hunting, deforestation and the trade of wildlife at markets can heighten the risk of diseases passing between animals and humans.
In 2018, a study warned of a possible link between deforestation in southeast Asia and a heightened risk of spillover of novel coronaviruses from bats to humans. The authors say:
Map showing the extent of deforestation in southeast Asia, with green showing tree cover and pink showing forest loss. Credit: Global Forest Watch“Owing to evolving land-use, bat populations are setting up in areas closer to human dwellings…This increases the risk of transmission of viruses through direct contact, domestic animal infection, or contamination by urine or faeces.”
A study published in April of this year looked into global drivers of mammal-to-human disease spillover, concluding:
“Our findings provide further evidence that exploitation, as well as anthropogenic activities that have caused losses in wildlife habitat quality, have increased opportunities for animal-human interactions and facilitated zoonotic disease transmission.”
It notes that “domesticated species, primates and bats were identified as having more zoonotic viruses than other species”.
The graph below, taken from the study, shows the relationship between virus richness and species richness for various mammal groups, including rodents, bats, primates, carnivores, artiodactyla (hoofed animals such as goats, sheep and giraffes), lagomorpha (hares, pikas and rabbits) and eulipotyphla (insect-eating mammals, such as hedgehogs, shrews and voles).
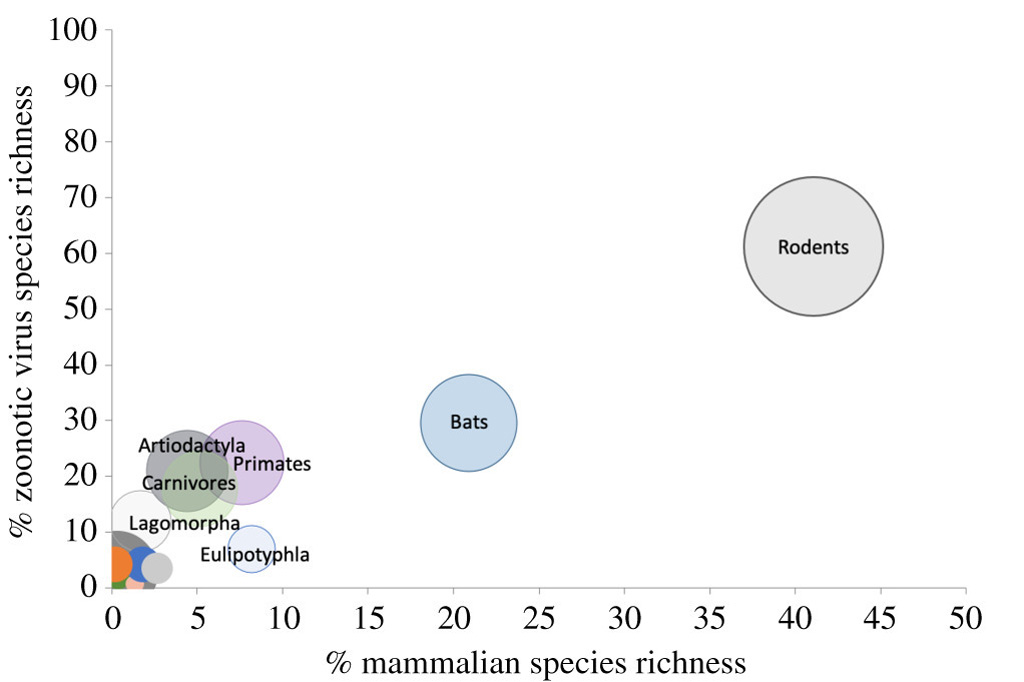
The graph shows how the rodent group contains both the highest number of different species and the highest number of different viruses. This is followed by bats and then primates.
It is worth noting that the impacts of climate change and biodiversity loss on disease spillover risk are likely to compound or moderate one another, says Redding.
For example, his research found that climate change could create more suitable habitat for Ebola-carrying bats. However, the degree to which this will translate into more disease spillover could depend on how humans interact with the animals’ new habitat in the future, he says:
“The numbers of people and how they are interacting with that land is probably going to dominate the more subtle effects.”
Both climate change and biodiversity disturbance could heighten spillover risk in the same way, by opening up new avenues between humans and animals, adds Poertner:
“It’s humans opening interfaces with nature that haven’t been there before and then you can get these encounters.”
Will the risk of animal-borne disease pandemics increase in the future?
Though research has uncovered links between climate change, biodiversity disturbance and disease spillover, it is still unclear how this could shape the future risk of pandemics, scientists tell Carbon Brief.
One major reason for this is scientists currently do not have a good understanding of how these pressures are affecting animal-borne disease risk at a global level, says Poertner:
“The major research priority now should be building some basic insight about how these [animal-borne viruses] will be changing under climate change. We have so many unknown viruses in the animal pool, it is important to identify those cases where crossing over may happen. But it’s like looking for a needle in a haystack.”
This point is echoed by IPBES authors Prof Josef Settele, Prof Sandra Díaz, Prof Eduardo Brondizio and Dr Peter Daszak who recently released a statement in response to the Covid-19 pandemic. They say:
“The potential for future pandemics is vast. As many as 1.7m unidentified viruses of the type known to infect people are believed to still exist in mammals and water birds. Any one of these could be the next ‘disease X’ – potentially even more disruptive and lethal than Covid-19.”

It is their opinion that pandemics will become more likely in the future if existing pressures on biodiversity continue. They say:
“Future pandemics are likely to happen more frequently, spread more rapidly, have greater economic impact and kill more people if we are not extremely careful about the possible impacts of the choices we make today.”
(UPDATE 30/10/2020: On 29 October, IPBES released a rapid workshop report detailing the links between the loss of nature and the emergence of novel diseases. The report found that future pandemics will “emerge more often, spread more rapidly, do more damage to the world economy and kill more people than Covid-19 unless there is a transformative change in the global approach to dealing with infectious diseases”. It also found that economic costs of tackling another pandemic would be around 100 times higher than the cost of prevention.)
In terms of climate change’s impact on animal-borne diseases, researchers still have a lot to learn, says Redding:
“We’re in a fairly embryonic stage of understanding this. People have been recently concentrating more on vector-borne diseases. There are far more zoonotic pathogens carried by mammals and birds than there are transmitted by insects, and we need to better understanding what impact climate change will have on this group .”
“Vector-borne diseases” are those spread by insects, such as malaria, dengue fever and Zika virus. Lots of research papers have shown that climate change could shift the range of such diseases, often further towards the poles.
For example, a study published in 2019 found mosquito-borne diseases could reach an additional one billion people by 2080, mostly in higher latitudes, if future global warming is extremely high.
By comparison, the impact of climate change on animal-borne diseases has been subject to very little research, says Redding. The WHO categorises the vast majority of animal-borne diseases as “neglected” because they “are not prioritised by health systems at national and international levels”.
In addition to better understanding how the pressures of climate change and biodiversity loss might affect animal-borne diseases, there is also a need to research the potential solutions, notes Poertner:
“A personal challenge that arises here for me is while all these dangers are imminent, there is an urgency to not only investigate the phenomenon, in terms of its basic science, but also to immediately investigate solution options.”
One step that should be taken is to improve the monitoring of animal-human interactions, says Redding:
“Routine monitoring is the key here. This is where scientists go out regularly and randomly monitor lots of people and their potential exposure to animals. This will have more of a ‘canary in the coalmine’ approach rather than a ‘by the time we’ve detected it, it’s too late’ approach.”
Such a monitoring system would demand a great level of global cooperation, Evengard says:
“We need to have a proper surveillance and also a monitoring system. But in order to have that, we really need to have very solid genuine international collaboration, involving the sharing of data and transparency. That’s really important.”
An organisation that could take on this responsibility could be the WHO, she adds.
Conserving existing wildspaces and restoring degraded ecosystems could also be an important step to protecting wildlife and people, says Poertner:
“We should not penetrate the last corners of the natural world. Biodiversity conservation has already produced the finding that 30% of land and 30% of the ocean should be set aside and left undisturbed in order for natural ecosystems to evolve and adjust to climatic changes that we are already imposing.”
It will also be important to address human activities that heighten the risk of disease spillover, including deforestation and the trade of wildlife, Redding adds:
“We need to have a better regulation of supply chains, which should include better accountability of how richer countries are often driving the demand for these activities.”
-
Q&A: Could climate change and biodiversity loss raise the risk of pandemics?
-
Climate change, biodiversity loss and pandemics: What does the science say?